What is frozen shoulder and how to get rid of it?

Frozen shoulder, medically known as adhesive capsulitis, is a common yet often misunderstood condition characterised by persistent pain and a marked restriction in shoulder movement. For many people, the gradual loss of the ability to lift a cup of tea, fasten a bra, reach a shelf, or even brush their hair can be both frustrating and alarming.
Although the condition can significantly interfere with daily life, understanding its causes, stages, and prevention strategies can make a meaningful difference. With early guidance, appropriate exercises, and professional support—including care from an experienced osteopath—most people recover well and regain functional movement.
Understanding Frozen Shoulder
Frozen shoulder affects the shoulder joint capsule, the strong connective tissue structure that surrounds and stabilises the joint. In adhesive capsulitis, this capsule becomes inflamed, thickened, and tight. Over time, adhesions may develop, limiting the joint’s natural mobility. As the capsule stiffens, both active movement (when you move your arm yourself) and passive movement (when someone else moves it for you) become restricted.
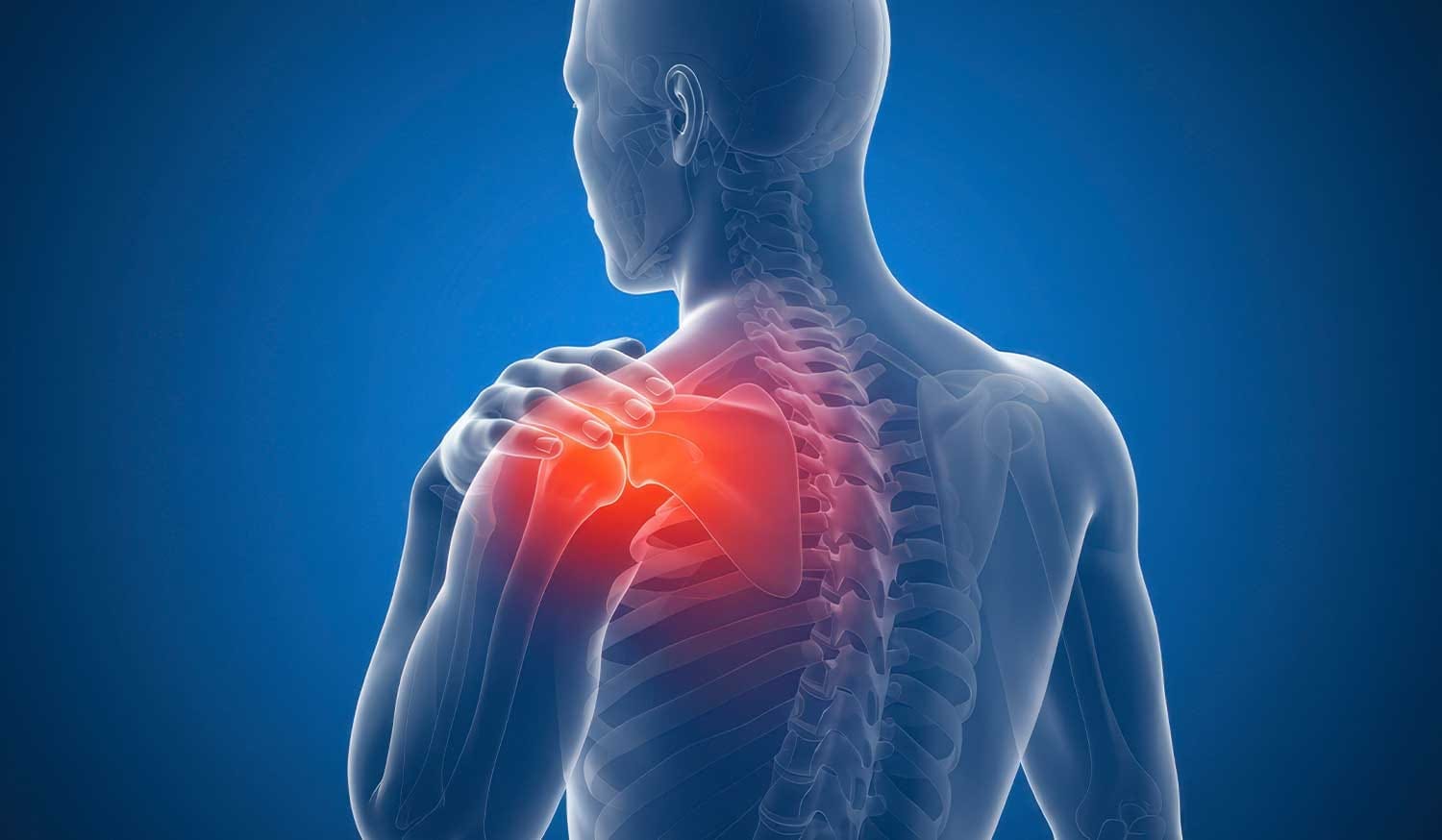
Although the precise pathological mechanism is still being researched, frozen shoulder typically progresses through three recognisable stages:
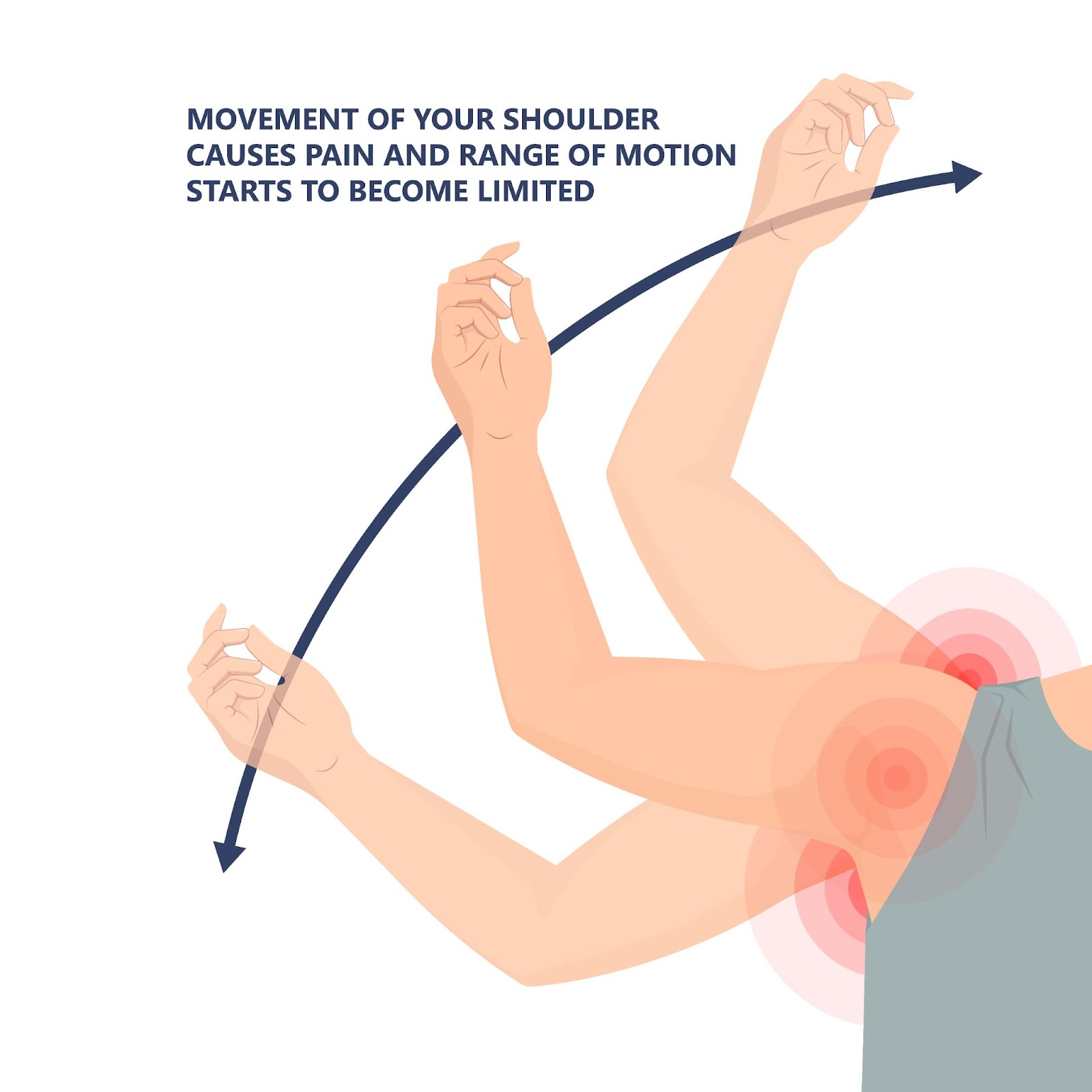
Freezing (Painful) Stage: This phase is characterised by a gradual onset of shoulder pain that worsens over approximately 6–9 months. The pain may be constant, often intensifying at night, and movement becomes increasingly limited.
Frozen (Stiff) Stage: During this stage, which usually lasts 4–6 months, pain may reduce slightly. However, stiffness remains severe, and the range of motion is significantly restricted. Everyday tasks such as dressing, driving, or reaching overhead can become particularly difficult.
Thawing Stage: In this final phase, mobility slowly improves over 6–12 months as the joint capsule gradually loosens. Function returns progressively, though patience is often required.
In total, the condition may take one to three years to fully resolve. While this timeline can feel discouraging, early intervention can help manage symptoms and potentially shorten recovery.
Medical Causes of Frozen Shoulder
Frozen shoulder can develop spontaneously, but several medical and physiological factors increase the likelihood of its onset.
Diabetes Mellitus
Individuals with diabetes are up to five times more likely to develop frozen shoulder compared to the general population. Elevated blood glucose levels can alter collagen structure within connective tissues, causing the shoulder capsule to thicken and lose elasticity. Both type 1 and type 2 diabetes are associated with increased risk.
Post-Surgical Immobilisation
After shoulder or chest surgery—such as rotator cuff repair, mastectomy, or certain cardiac procedures—prolonged immobilisation can trigger adhesive capsulitis. When the joint is not moved regularly within a safe range, the capsule may contract and stiffen around the joint.
Trauma and Injury
Significant shoulder trauma, including fractures, dislocations, or soft-tissue injuries, can lead to inflammation within the joint capsule. In some cases, excessive scar tissue formation contributes to long-term stiffness and restricted movement.
Thyroid Disorders
Both hypothyroidism and hyperthyroidism have been linked to a higher incidence of frozen shoulder. Hormonal imbalances may influence collagen metabolism and connective tissue health, increasing susceptibility to capsular tightening.
Cardiovascular Disease
Emerging research suggests a possible association between cardiovascular conditions, such as heart disease or stroke, and frozen shoulder. Reduced activity levels and vascular changes may contribute to this connection, although further studies are ongoing.
Lifestyle-Related Risk Factors
In addition to medical triggers, several lifestyle factors can increase the likelihood of developing frozen shoulder.
Sedentary Behaviour
Spending prolonged periods sitting at a desk or using digital devices can reduce shoulder mobility. Lack of regular movement encourages stiffness and poor joint mechanics.
Poor Posture
Rounded shoulders and forward head posture place sustained stress on the shoulder complex. Over time, this may contribute to micro-trauma and capsular irritation.

Smoking
Nicotine negatively affects circulation and tissue healing. Impaired microcirculation may exacerbate capsular fibrosis and delay recovery.
Obesity
Excess body weight is associated with systemic inflammation and a higher prevalence of musculoskeletal disorders, including adhesive capsulitis.
Addressing these factors proactively can significantly reduce risk and improve overall musculoskeletal health.
The Role of Osteopathy in Prevention and Management
Osteopathy takes a holistic approach to musculoskeletal care. Rather than focusing solely on the shoulder joint, osteopaths assess the entire body, including posture, spinal alignment, biomechanics, and lifestyle influences.
Comprehensive Assessment
An osteopath will evaluate shoulder mechanics, posture, range of motion, and contributing health conditions. Identifying underlying risk factors is essential for tailored care.
Manual Therapy
Gentle articulation, mobilisation, and myofascial release techniques may help reduce pain and improve capsule flexibility. Treatment is always adapted to the individual’s tolerance and stage of the condition.
Exercise Prescription
Targeted stretching and strengthening exercises are central to recovery. Carefully designed programmes aim to maintain mobility, support joint stability, and prevent recurrence.
Lifestyle and Ergonomic Advice
Adjustments to workstation setup, posture correction strategies, and activity modification can reduce strain on the shoulder joint.
Holistic Health Support
For individuals with diabetes, thyroid disorders, or other systemic conditions, osteopaths may provide guidance that complements medical management, including advice on physical activity and healthy habits.
Osteopaths in the UK are regulated by the General Osteopathic Council (GOsC) and must adhere to evidence-based practice standards. This ensures that patient care remains safe, ethical, and professionally accountable.
Prevention Strategies to Reduce Risk
Although not all cases of frozen shoulder can be prevented, several practical strategies can lower your risk:
Maintain Regular Shoulder Movement
Perform gentle shoulder circles, pendulum swings, and wall-walking exercises daily—especially if recovering from injury or surgery.
Incorporate Strength and Flexibility Training
Exercises such as doorway chest stretches, cross-body arm stretches, and resisted external rotations help preserve capsule elasticity and shoulder stability.
Optimise Ergonomics
Ensure your workstation supports good posture. Keep your monitor at eye level, shoulders relaxed, and elbows supported. Take short breaks every 30 minutes to stretch.
Manage Underlying Conditions
If you have diabetes or thyroid disease, regular medical check-ups and optimal condition management can reduce connective tissue complications.
Early Post-Operative Mobilisation
After surgery, follow rehabilitation protocols carefully. Gentle, guided movement within a pain-free range helps prevent capsular tightening.
Adopt Healthy Lifestyle Habits
Quitting smoking, maintaining a healthy body weight, and following an anti-inflammatory diet rich in omega-3 fatty acids may support connective tissue health.
When to Seek Professional Advice
It is advisable to consult a healthcare professional if you experience persistent shoulder pain lasting more than six weeks, progressive stiffness, difficulty lifting your arm overhead or behind your back, or worsening night pain. Numbness, tingling, or weakness should also be assessed to rule out other conditions.
Early assessment allows for accurate diagnosis and appropriate management, potentially preventing long-term limitation.
The Reassuring Outlook
Despite its slow progression and frustrating symptoms, frozen shoulder almost always resolves over time. While recovery may take months or even years, consistent care, guided exercises, and professional support can significantly improve comfort and function. With patience and proactive management, most individuals regain near-normal shoulder movement and return to their usual activities.
Understanding the condition, addressing risk factors, and seeking early guidance are the most effective steps you can take to protect your shoulder health and maintain long-term mobility.





